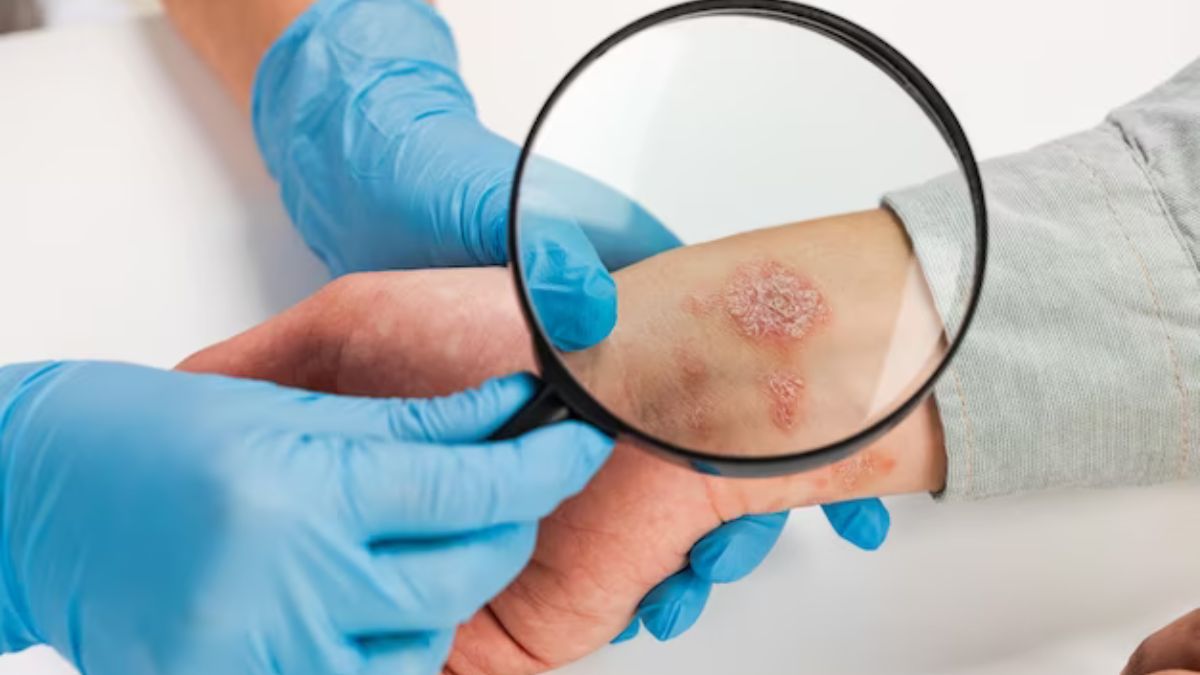
Hidradenitis Suppurativa (HS) is a chronic skin illness that affects the armpits, groin, and buttocks and results in itchy pimples, boils, abscesses, and scars. These symptoms can be quite painful and are often chronic. It affects the armpits, groin, and breasts but can also occur in other body areas.
It can lead to isolation and a poor quality of life, but getting diagnosed early and managing symptoms with a treatment plan is possible. Understanding the different stages can help people feel more prepared and empowered to seek treatment.
Stage 1: Nodules
A person with HS develops painful, pus-filled nodules and abscesses (also called lesions) in the skin. The disease often starts in the groin and pubic area but can also affect other body parts. The cause isn’t known. However, it may be linked to hormones and genetic predisposition. They also suggest that cigarette smoking and excess weight play a role.
During an HS flare-up, the nodules might break open and drain pus with an unpleasant odor. Gentle washing with antiseptic soap can help reduce the odor. Medications like antibiotics and painkillers might be prescribed to control the inflammation and ease pain. These drugs might be given as creams, tablets, or liquids. Common antibiotics used for HS include lymecycline, doxycycline, and erythromycin. A retinoid medicine, such as acitretin, can also be effective.
Because hidradenitis suppurativa can look like pimples or acne, getting a diagnosis and treatment might take a while. A person with skin conditions may be referred to a dermatologist after seeing other clinicians, such as family medicine, internal medicine, pediatricians, or gynecologists.
The underlying reason behind hidradenitis suppurativa is not fully comprehended, but it is a self-inflammatory disorder that targets the hair follicles, leading to uncomfortable nodules and abscesses. It is not a result of poor hygiene, nor can it be spread to other people. With timely treatment, your quality of life can be significantly improved even though the condition may persist for an extended time.
Stage 2: Abscesses
HS can cause painful boil-like lumps to form under your skin in places where your body’s fat and sweat glands rub together, such as your armpits or groin. When these lumps rupture, they create a swollen area that drains pus. These sores are called abscesses. They can be painful, itchy and smelly. They can also get infected and lead to scarring. People with a weak immune system get these abscesses more often than others.
Doctors don’t know what causes hidradenitis suppurativa. They think it combines genes, hormones, and the environment. It’s more common in women than men and usually starts between puberty and age 40, most often between ages 21 and 29. It runs in families. It’s not caused by poor hygiene.
The exact cause isn’t known, but the hair follicles are believed to become blocked. Hormones are thought to play a role, as well as being overweight and smoking. Having a family history of the condition makes it more likely to develop.
Therapy can help you properly manage your Hidradenitis Suppurativa symptoms, even if no known cure exists. A dermatologist may recommend benzoyl peroxide, chlorhexidine, or zinc pyrithione-based medicated washes. You can also use antibacterial ointments or creams to keep the sores clean. Injections of the immunosuppressant drugs infliximab and adalimumab can help reduce flare-ups.
Stage 3: Tunnels
During this stage, people with HS develop long, thin tunnels under the skin, which are often draining. These tunnels are surrounded by inflammation and may be painful to touch. The disease is also more severe at this stage, causing widespread abscesses and sinus tracts throughout the body.
Compared to skin without tunnels, histologically confirmed tunnel samples showed higher expression of pro-inflammatory cytokine mRNA. Elevated expression of keratinocyte-derived factors (S100A7, S100A8, and S100A9) and antimicrobial factors (DEFB4, IL-26) was consistent with the epithelized nature of the tunnels. Additionally, lipocalin-2 staining demonstrated neutrophil solid infiltration of the lumen of tunnels.
At this stage, HS has spread to multiple areas of the body, including the axillae, neck, and inframammary folds, as well as the groin, mons pubis, vulva, perineum, and genital area. People with HS at this stage experience a poorer quality of life than those in the mild and moderate stages of the condition.
During this stage, people with HS experience chronically infected and draining lesions on their bodies that never fully heal. They have difficulty moving around and may have a limited diet due to the presence of open wounds. The damage to the lymphatic system can also complicate symptoms. The disease can cause the lymphatics to get blocked, resulting in fluid build-up and edema.
Stage 4: Scars
Hidradenitis suppurativa (hi-drad-uh-NIE-tis sup-puh ruh-TIE-vuh) is a long-term (chronic) condition that causes painful, inflamed areas with chronic drainage and scarring. It often starts in places where your skin rubs together, like the armpits, groin area, buttocks, or breasts. It is not contagious. It usually starts after puberty and can recur for years. It can cause emotional and physical distress. It can also affect your work and personal relationships. Combined medical and surgical treatment can help manage symptoms.
HS is more common in women than men and tends to start during the teen or early twenties, but it can happen at any age. Scientists are still trying to pinpoint the precise etiology of HS, although many variables, including genetics, hormones, and the environment, may have an impact. Evidence suggests that smoking and obesity may contribute to the development of HS, which appears to be more prevalent in the African-American community than in white populations.
The first step in treating HS is to use antibiotics to reduce inflammation. You’ll need to take them for at least three months, and they may be a cream, tablet, or injection. If your condition is severe, you might need a more muscular type of steroid, such as prednisolone or another steroid. You may also be given a medication that suppresses your immune system to prevent flares, such as adalimumab or infliximab. Still, these medicines are only used if other treatments don’t work.